Introduction: Coding a GI cocktail (e.g. Maalox + lidocaine + anticholinergic) can be tricky. There’s no dedicated CPT/HCPCS code for this oral mixture, so it’s often bundled into the office/ER visit. As a result, practices frequently face claim denials or write-offs. This guide (from GenMediTech’s billing experts) explains current coding rules and shows how to maximize reimbursement for GI cocktails. We include ICD-10-CM/CPT guidance and step-by-step examples so you can bill correctly and avoid revenue leakage.
What Is a GI Cocktail in Billing?
A GI cocktail is an oral mixture (antacid, viscous lidocaine, and an anticholinergic like donnatal) used for GI pain relief. Because it’s not an FDA-approved drug product with a fixed formula, coders must treat it as a composite service. This ambiguity arises because GI cocktails are self-administered oral drugs – CMS explicitly excludes drugs typically taken by patients. In practice, this means oral GI cocktails are usually not reimbursed separately. Instead, they’re considered part of the Evaluation & Management (E/M) service (doctor’s visit) unless an alternate code is justified.
Official Coding Rules & Coverage
- CPT/HCPCS Basics: No CPT code exists for a “GI cocktail.” By CPT convention, treatments like medication administration during a visit are bundled into the E/M code. The AMA CPT guidelines state that most physician services (including in-office treatments) are included in E/M codes.
- HCPCS Drug Codes: Some practices attempt HCPCS codes for GI cocktail ingredients. For example, J8499 (Oral, non-chemotherapy drug) or J3490 (Unclassified drug) might be used for lidocaine or other ingredients. Similarly, CPT 99070 (supplies) is sometimes tried for the antacid portion. However, carriers often deny 99070 for GI cocktails, labeling it a medication-related supply.
- Medicare (CMS) Policy: Medicare classifies oral medications (like a GI cocktail) as usually self-administered. Thus, Medicare Part B won’t pay separately for a GI cocktail; you bill only the appropriate E/M code. Commercial insurers often follow this logic, so attempted coding of oral cocktail components generally fails.
- Bundling (NCCI): The CMS NCCI policy (updated annually) implies that “ancillary” services are bundled into primary codes. In GI cocktail billing, this means everything – aside from the visit – is normally bundled. Expect payers to bundle the cocktail cost into the E/M payment unless you bill an unlisted code with justification.
Step-by-Step GI cocktail Coding Workflow
Use this workflow to decide how to code a GI cocktail for any encounter:
- Confirm Scenario & POS: Identify the setting and reason for visit. (e.g. Urgent Care uses CPT 99202–99205, ER uses 99281–99285). The setting dictates which code set you use.
- Bill the E/M Visit: Assign the appropriate E/M code based on MDM/time. The GI cocktail is typically included in this code’s payment. Do not upcode E/M just because you gave a cocktail – follow the AMA’s E/M documentation rules.
- Consider Drug/Supply Codes: If any GI cocktail components were administered via injection (rare, but e.g. IV lidocaine), you could add CPT 96372 (therapeutic injection). For oral ingredients, no separate code applies.
- Alternate Codes (99070/J-codes): If you pursue separate billing, CPT 99070 (supplies) or a HCPCS code can be attempted. For example, J8499 might be billed for lidocaine if documented (though oral lidocaine is often denied). Remember, payers often reject 99070 for cocktails.
- Unlisted Codes: If needed (and only after denials), use an unlisted procedure code with full documentation. Examples: 44799 (unlisted intra-abdominal) or 90799 (unlisted immunization). Attach a detailed note justifying why no standard code applies. This is a last resort; success depends on payer review.
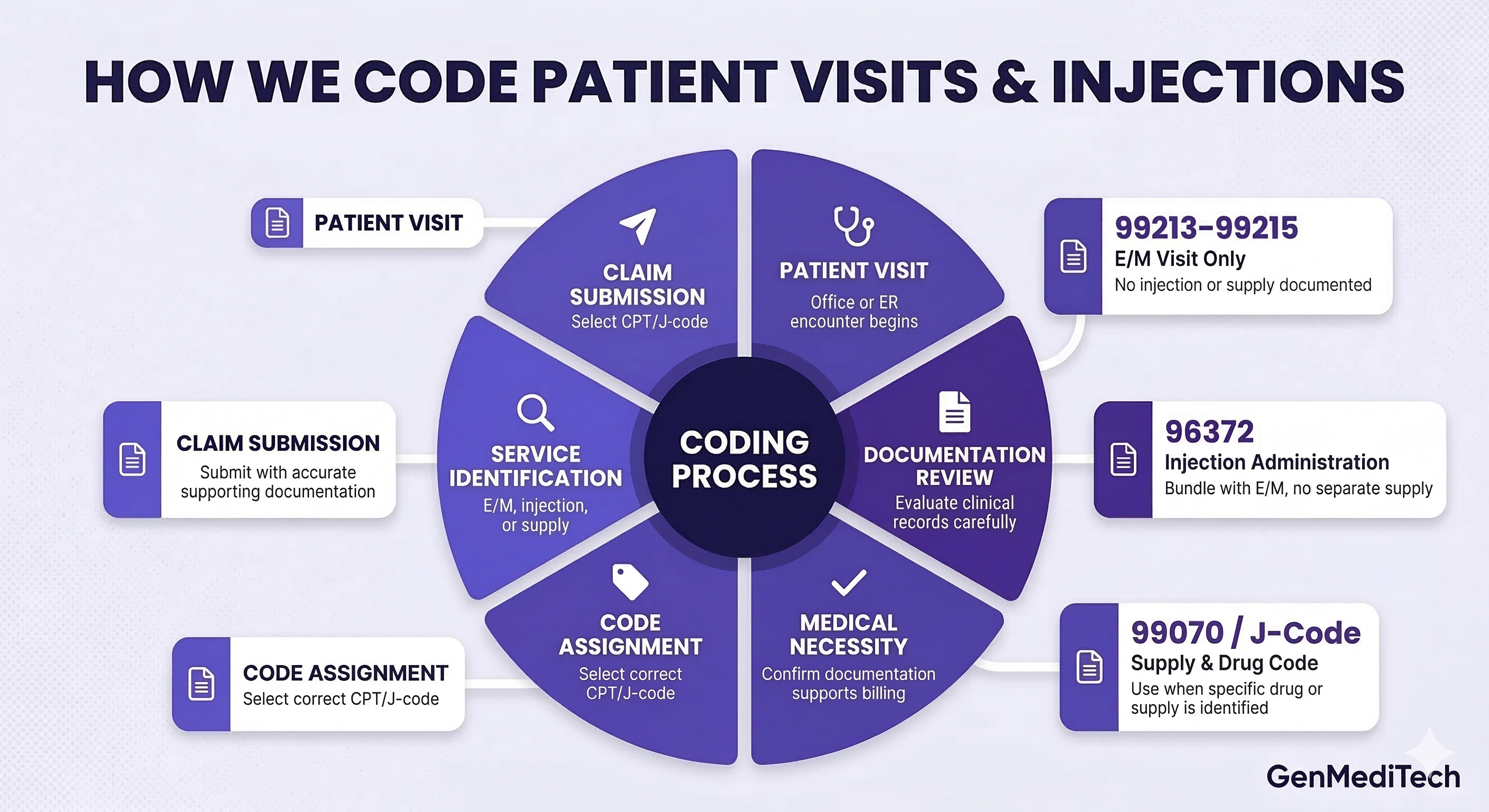
This chart shows key decision points: mostly E/M, rarely injections or alternate codes
Billing Scenarios & Examples
| Scenario | Billing Strategy | Coding Notes |
|---|---|---|
| Urgent Care Visit (99202) with oral GI cocktail: | Bill 99202 only. | Cocktail cost is bundled. (No extra code is needed.) |
| ER Visit (99284) with IV antiemetic + oral GI cocktail: | Bill 99284 + 96372 (for IV lidocaine) | Oral cocktail still bundled; 96372 covers the injection. |
| Billing 99070 for Cocktail: A practice uses 99070 + E/M. | Claim is usually denied. | Carriers often say 99070 isn’t valid for oral meds. |
| Medicare Enrolled Patient: | Bill standard E/M code only. | GI cocktail (oral) is non-covered by Medicare. |
| After Denial – Unlisted Code: | Bill 44799 with detailed note. | Example: “No specific code for oral analgesic mix; see documentation.” |
(For example, if Medicare denies J8499, only the visit code remains payable. We cite CMS’s exclusion to support this.)
Documentation & Denial-Prevention
- Document Everything: Note patient symptoms (e.g. “abdomen pain, suspected gastritis”), all cocktail ingredients and doses, and why it was given (e.g. “diagnostic relief prior to endoscopy”). Clear records justify coding choices.
- E/M Based on MDM/PE: Use CMS’s and AMA’s E/M guidelines to set the code. Do not bump the E/M level by citing the cocktail – follow true MDM/time criteria.
- Appeals Tips: If a cocktail-related claim is denied, appeals should emphasize medical necessity: e.g. “Medication mix was essential for patient management.” Attach copies of clinical notes and reference that GI cocktails lack a specific code.
- Payer Notes: Medicaid rules vary; always verify with local Medicaid manuals. Commercial policies often mirror Medicare’s self-administered drug exclusion.
- GenMediTech Tip: Our billing staff uses internal “GI Cocktail Justification” templates when filing unlisted codes, to meet payer requirements. Having this play ready speeds up appeals.
FAQs (Optimized for Featured Snippets)
Q: Is there a GI cocktail CPT code?
A: No. GI cocktails (an oral antacid/viscous lidocaine mix) have no specific CPT code. They are treated as part of the E/M service.
Q: Can I bill CPT 99070 or J8499 for a GI cocktail?
A: You can try, but these often fail. CPT 99070 (supplies) is typically denied for medication contents. J8499 (oral drug) may be used for lidocaine, but Medicare’s rules exclude it if taken orally.
Q: Will Medicare pay for a GI cocktail?
A: Generally no. Medicare excludes drugs usually self-administered. Since a GI cocktail is taken orally by the patient, Medicare won’t reimburse it separately – only the doctor’s visit can be billed.
Q: When should I use an unlisted code?
A: Only if no standard code fits. For example, if all attempts (99070, J-codes) are denied, you might use an unlisted CPT (with full documentation) to attempt reimbursement.
Q: Which E/M code covers GI cocktail visits?
A: Bill whichever E/M code matches your encounter (e.g. 99202 in urgent care or 99284 in ER). The GI cocktail has no separate code, so it’s included.
Q: How to document GI cocktail billing?
A: List each medication/amount, note the diagnosis/problem it treats, and record the patient’s response. This supports any code you bill and aids in any appeals.
Conclusion
Proper coding of GI cocktails hinges on understanding bundling rules and payer policies. In almost all cases, the cocktail’s cost is included in the visit’s E/M code. Attempting separate codes (99070, J3490, J8499, unlisted) can be done, but expect denials. If coding complex cases is a challenge, GenMediTech’s billing experts are here to help your practice. We offer medical billing and consulting services that ensure every billable service (like GI cocktails) is handled correctly to maximize revenue. Contact GenMediTech for a free RCM review and see how we can streamline your billing process.



